With the advancement of billing in every medical specialty, the field of billing in psychiatry and billing for mental health services is most significantly impacted. As the financial management of the behavioral health practice gets a more pronounced role due to increasing demand for mental health services and the complexity of the service, the awareness and demand for services are paradoxically increasing.
Research indicates that approximately 30% of behavioral health claims get denied on the first submission, in contrast to 19% in the rest of the medical specialties, which indicates the complexity of mental health billing.
Behavioral health claims are reported to have a 15 to 20 % claim denial rate, which is higher compared to the general medical billing and is attributed to a lack of documentation, coding errors, and authorization errors.
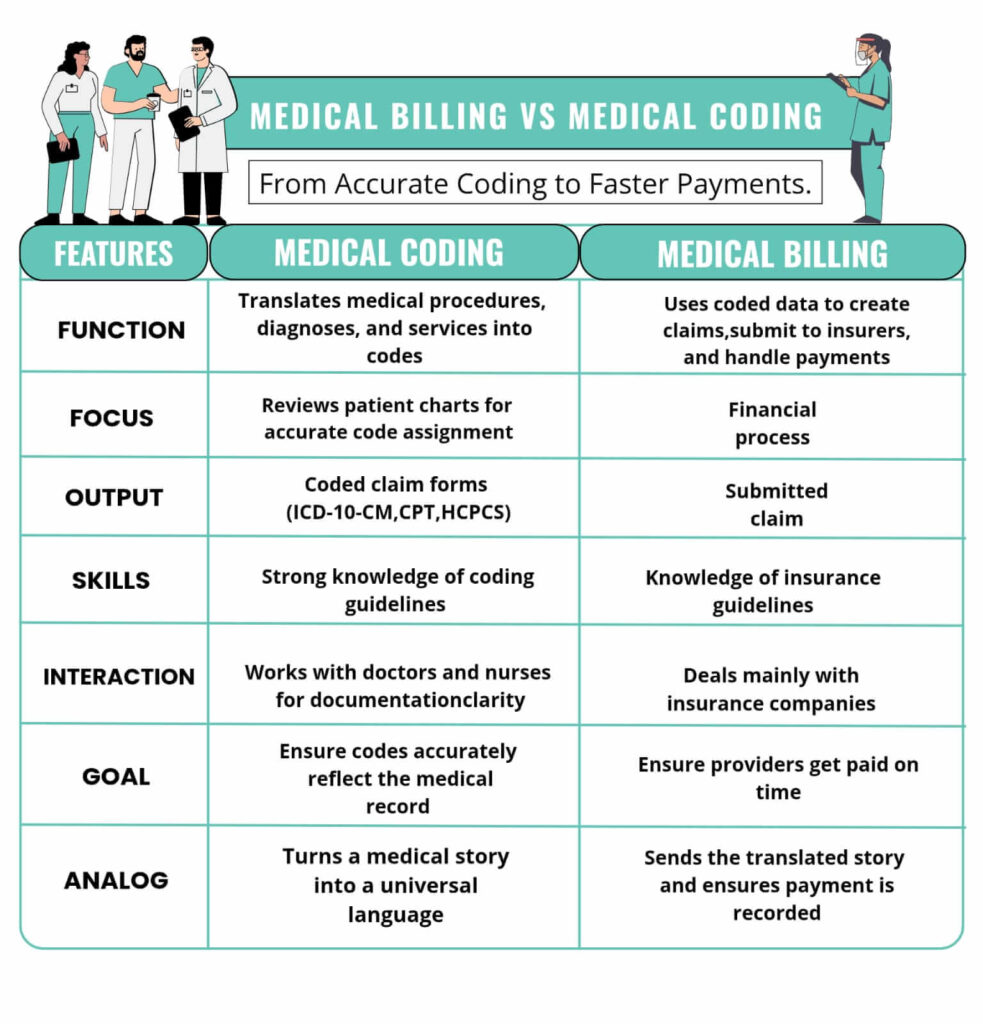
How Is Mental Health Billing Different From Medical Billing?

Mental health billing and general medical billing may appear similar to you. Because both rely on CPT and ICD-10 codes. However, mental and behavioral health billing operates under very different reimbursement structures, documentation standards, and payer rules.
These differences require specialized billing expertise to avoid denials, audits, and compliance issues.
Below are the key factors that distinguish mental health billing from general medical billing.
1. Time-Based Billing vs. Procedure-Based Billing
In general medical billing, services are typically procedure-based. A specific CPT code corresponds to a defined service such as a lab test, imaging study, or surgical procedure, regardless of time spent.
In mental health billing, many services, especially psychotherapy, are time-based. CPT codes are selected based on actual minutes spent with the patient.
This makes accurate time tracking essential, which is not usually required in most medical specialties.
2. Preauthorization and Coverage Restrictions
Preauthorization is far more common in behavioral health than in general medical billing.
- Many insurers require prior authorization before therapy begins
- Authorization is often limited by:
- Number of sessions
- Length of treatment
- Diagnosis severity
- Medical services such as labs or office visits often do not require ongoing authorization
Failure to obtain or renew authorization is one of the leading causes of mental health claim denials.
3. More Complex Documentation Requirements
Mental health billing requires extensive narrative documentation, not just procedural notes.
Documentation must demonstrate:
- Medical necessity
- Treatment goals
- Interventions used
- Patient response
- Measurable progress over time
- Justification for continued care
In contrast, most medical billing relies on problem-focused or procedure-based documentation, which does not require continuous progress justification.
4. Staffing and Practice Structure Challenges
Many mental health practices are:
- Solo providers
- Small group practices
- Therapy-focused clinics
Unlike large medical practices that employ dedicated billing departments, behavioral health providers often:
- Handle their own billing
- Rely on limited administrative staff
- Outsource billing more frequently
This increases the risk of coding errors and missed compliance requirements.
5. Coding Complexity and CPT Variability
Behavioral health billing involves:
- Multiple CPT code families
- Time thresholds
- Provider-specific billing rules
- Add-on codes (e.g., psychotherapy with E/M)
Codes vary based on:
- Length of session
- Type of service
- Provider credentials (psychiatrist vs therapist)
- Individual vs group vs family therapy
General medical billing tends to be more standardized and less variable.
6. Frequency Limits and Session Caps
Mental health services are commonly subject to:
- Annual session limits
- Medical necessity reviews
- Frequency restrictions (e.g., once per week)
These limitations are far less common in medical billing, where procedures are usually approved per occurrence.
Insurers may deny claims once a session cap is reached. Even if treatment is clinically necessary.
7. Ongoing Medical Necessity and Progress Tracking
In mental health billing, medical necessity must be continuously proven, not just established once.
Providers must:
- Show measurable improvement
- Update treatment plans
- Justify continued therapy
- Modify interventions if progress plateaus
In most medical billing scenarios, once a service is authorized and performed, ongoing justification is not required.
8. Higher Risk of Claim Denials and Audits
Mental health claims are denied more frequently due to:
- Missing or expired authorizations
- Insufficient documentation
- Time-based coding errors
- Inconsistent progress notes
Psychotherapy claims, in particular, are subject to post-payment audits, making compliance critical.
Key Differences Between Mental Health Billing and Medical Billing
Here’s a summarized comparison of the most significant differences:
| Feature | Medical Billing | Behavioral & Mental Health Billing |
| Billing Basis | Procedure & service | Time-based & therapy-specific |
| CPT Coding | Standardized for most procedures | Variety of psychotherapy codes |
| Documentation | Brief and focused | Detailed progress notes required |
| Insurance Coverage | Fewer limits | Often caps on sessions & requires preauth |
| Staffing | Usually dedicated teams | Often clinician-managed |
Sources show that mental health claims are denied more frequently than other medical claims due to these complexities and documentation requirements.
Why Specialized Billing for Mental Health is Important?
Mental health providers often have to deal with more claim denials and fewer reimbursements, compared to most medical specialties.
Industry data suggests that:
- Behavioral health claims have a 20%-30% higher rate of denials.
- Denials can occur due to insufficient documentation, incorrect CPT codes, or missing preauthorizations.
All of these factors put stress on the clinic’s cash flow, its staff, and its sustainability…
The Future of Mental Health and Medical Billing!

Medical billing for mental health services is more challenging than ever. It is because of the telehealth boom, changing payer policies, and new regulations, including parity laws.
So the practices are turning to automated RCM (revenue cycle management) strategies, which aim to make claim processing more efficient, accurate, and denial-proof.
Practices are turning to outsourcing medical billing services for mental health billing to make their revenue cycle better.
Choose Health & Billing for Psychiatric Billing Services
Mental health billing requires far more than basic medical billing knowledge.
The expert specialty-focused team at Health & Billing specializes exclusively in psychiatric and behavioral health billing. Thus, helping providers reduce denials. Stay compliant and maximize reimbursements, without the administrative burden.
We work with psychiatrists, psychologists, therapists, and behavioral health facilities, delivering billing solutions. That aligns with the unique complexities of mental and behavioral healthcare.
Our Psychiatric Billing Expertise Includes:
✔ Accurate & Compliant Coding
We ensure precise CPT and ICD-10 coding. Aligned with the latest payer and regulatory requirements. Including time-based psychotherapy, E/M services, and psychiatric evaluations.
✔ Documentation Support for Medical Necessity
Our team assists with documentation standards. To support medical necessity, treatment goals, progress tracking, and audit readiness, critical for behavioral health reimbursement.
✔ Denial Management & Resubmission Strategies
We proactively identify denial patterns, correct errors, and manage timely appeals. to recover lost revenue and prevent repeat denials.
✔ Telehealth & Virtual Care Billing
From telepsychiatry to teletherapy, we manage modifiers, place-of-service rules, and payer-specific telehealth requirements to ensure compliant virtual billing.
✔ Behavioral Health-Focused Reporting & Analytics
Gain clear insightsinto revenue trends, denial rates, authorization status, and payer performance with customized, easy-to-understand reports.
Why Health & Billing?

→ Specialized focus on mental and behavioral health billing.
→ Understanding of time-based and authorization-driven services.
→ Reduced claim denials and faster reimbursement cycles.
→ Scalable solutions for solo providers and multi-location practices.
→ Dedicated billing experts who understand psychiatric workflows.
Focus on Patient Care, We’ll Handle the Billing!
Let Health & Billing manage the complexities of psychiatric billing. While you focus on delivering high-quality mental health care. Our specialized billing solutions are designed to protect your revenue, ensure compliance, and support long-term practice growth.
→ Contact Health & Billing today to streamline your psychiatric billing operations.
FAQs
Why is mental health billing more complex than medical billing?
Mental health includes billing for time and attention spent on preparing and documenting time-based CPT codes, which detail specific services that limit the standardization of the claim, making it more likely to get denied.
How does telehealth affect mental health billing?
For telehealth, you have to deal with additional codes and modifiers specific to telehealth, and you need to document to the level of detail required to qualify for reimbursement, which complicates billing for behavioral health services even more.
Why do mental health claims get denied more often? Should psychiatry practices outsource billing?
The aforementioned MoAs (Missing, out of place, or inadequate Sections) are the reasons or contributing factors for the high rejection rates in telehealth mental health billing.
Should psychiatry practices outsource billing?
Most psychiatry and behavioral health practices find it useful to outsource billing to specialists, as it helps with the accuracy, speed, and reduction of denials, which helps processes.
How can I choose the right behavioral health billing outsourcing partner?
Consider their understanding of time-based coding, their denial management practices, the transparency of their reports, and their familiarity with mental health and telehealth billing.
How important is time documentation in mental health billing?
Because of the correlation of the majority of the psychotherapy CPT codes to the session duration, accurate time tracking is key. Errors can result in future denials or lower payments.