Billing can easily be daunting when a practice has to deal with procedure-heavy treatments, paperwork requirements, and continuous amendments in insurance regulations.
The economic cost is also significant. It has been found that approximately 1 out of 10 medical claims is initially denied. Moreover, the rates of denials increase even further because of the complicated procedure and the code requirements.
Lack of a structured billing process can expose practices to delayed payment, compliance problems, and loss of revenue. It is why it is necessary to learn the details of pain management and medical billing, both by the provider and the billing teams.
What Is Pain Management Medical Billing?

Pain management medical billing refers to the process of filing and processing claims for services that are to be offered in the diagnosis and treatment of chronic or acute pain conditions. Such services usually comprise:
- Epidural steroid injections.
- Nerve blocks
- Radiofrequency ablation
- Surgeries on spinal cord stimulators.
- Follow-ups and drug administration.
The medical billing pain management specialty has very strict requirements in billing and use of CPT, ICD-10, and HCPCS codes and documentation to demonstrate medical necessity. Coding mistakes will result in rejection or delays of claims, even when those mistakes are minor.
Why Pain Management Billing Is Complex?
The billing of pain management is not as simple as most specialties since it involves procedures, medication, and long-term plans in the treatment process of the same patient.
Many factors contribute to this complexity:
Multiple Procedure Codes
Most of the treatments involve more than one CPT code and a modifier. The loss of one of them can result in the rejection of claims.
Frequent Prior Authorizations
The insurance companies usually need prior authorization before any operation is done. Prior authorization is a problem that results in 25% of claims being denied in specialty care.
Formidable Paperwork Demands
The providers are required to record the history of the patient, image findings, history of treatment, and justification of the procedure account.
Changing Payer Policies
Payers’ rules and coding pain management medical billing guidelines are constantly evolving, which entails constant updates and training.
As a result of these factors, up to 30% of the potential revenue is lost as a result of billing errors and denials associated with some of the pain management practices.
Key Components of Pain Management Medical Billing

Effective medical billing pain management requires a number of processes linked together in the revenue cycle.
→ Checking of Patient Eligibility and Insurance
Insurance verification should be done before the appointment, as this would prevent claims being denied due to eligibility mistakes- one of the most frequent causes.
→ Accurate Medical Coding
Coders have to have the right procedure and diagnosis codes based on documentation. The major proportion of rejected claims in the specialty of medical billing for pain management is due to incorrect or outdated coding.
→ Pre-authorization Administration
There is a high number of treatments that are pre-approved, such as injections and neurostimulation procedures. Lack of authorization is one of the causes of claim denial.
→ Charge Capture
Getting all the billable services means practices will not lose money. Research indicates that the charge capture is effective in minimizing revenue leakage by 5-10%.
→ Submission and Follow-Up of Claims
With fast payment and frequent monitoring of clean claims, the reimbursement schedules are enhanced, and the time spent on accounts payable is shortened.
Pain Management Billing and Coding Process: Step by Step
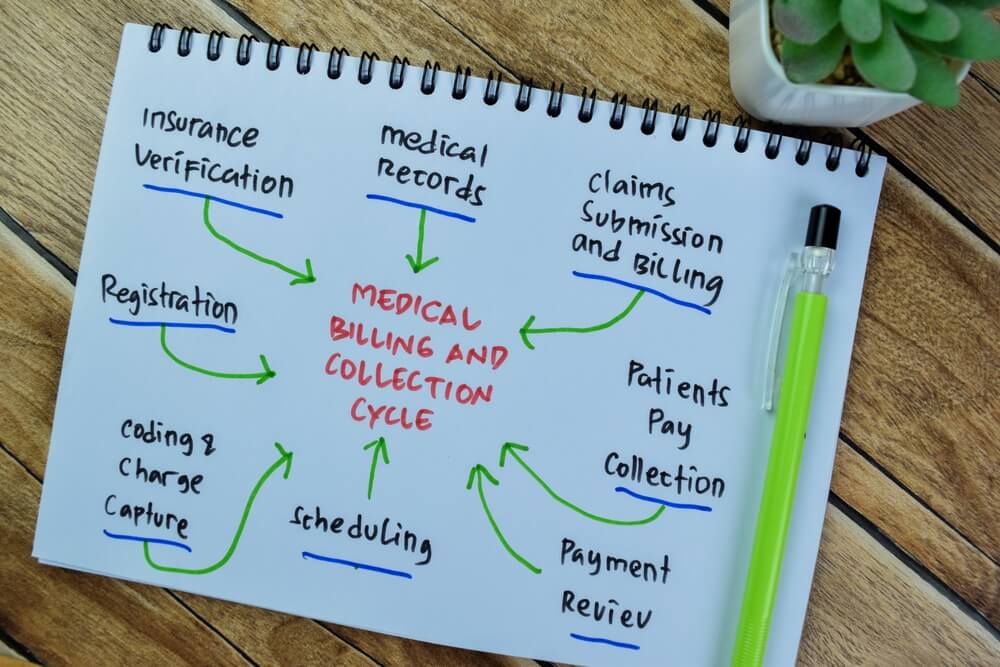
Measurement of a workflow enables the minimization of errors and the enhancement of revenue performance. The following is a step-by-step procedure for successful medical billing for pain management practices.
Step 1: Patient Registration
Demographic and insurance information regarding patients is gathered and checked before the provision of services.
Step 2: Verification and Authorization of Insurance
The billing department verifies the benefits and receives prior authorization in case of need.
Step 3: Medical Documentation
Providers record symptoms, treatment history, imaging findings, and the procedure performed.
Step 4: Coding the Services
Medical coders make correct CPT, ICD-10, and modifiers depending on the documentation.
Step 5: Assertion and Filling of a Claim
Claims are filed online with the insurance companies following claims scrubbing checks carried out internally.
Step 6: Payment Posting
Insurance/patient payments are captured and counterbalanced with Explanation of Benefits (EOBs).
Step 7: Management of Denial and Appeals
Rejection of claims is checked and reworked, and resubmitted. With the management of denials, 60-70% of the rejected claims can be recovered.
Common Pain Management Billing Challenges

Pain management is considered one of the most complex specialties in medical billing due to high regulatory scrutiny, frequent audits, and strict documentation requirements.
Despite following standard billing procedures, many practices encounter recurring challenges.
1. High Claim Denials
Claim denials remain a major concern across the healthcare industry.
Industry reports indicate that average denial rates have hovered around 10-20% in recent years, and they continue to rise.
Pain management claims are especially vulnerable due to:
- Medical necessity scrutiny.
- Frequency limitations on injections.
- Bundling edits.
- Missing prior authorizations.
Remember! Even small documentation gaps can trigger denials.
2. Coding and Modifier Errors
Pain management procedures often require precise CPT coding and correct modifier usage (such as modifiers for bilateral procedures, multiple procedures, or distinct procedural services).
Common coding issues include:
- Incorrect injection level reporting.
- Failure to append appropriate modifiers.
- Unbundling or bundling errors.
- Mismatch between ICD-10 diagnosis and CPT procedure.
These mistakes frequently result in delayed reimbursements or outright claim rejections.
3. Prior Authorization Delays
Many interventional pain procedures require prior authorization. It is to be done from insurance carriers.
Failure to obtain timely approval can result in automatic denials.
Authorization challenges include:
- Frequent payer-specific requirements.
- Imaging documentation requests.
- Conservative treatment proof requirements.
Delays can disrupt cash flow and patient scheduling.
4. Strict Medical Necessity Documentation
Pain management billing heavily depends on strong documentation to justify treatment.
Insurers often require documentation of:
- Pain duration.
- Functional limitations.
- Failed conservative therapy.
- Imaging results.
- Response to prior injections.
Insufficient documentation increases the risk of audits and recoupments.
5. Regulatory Compliance & Audit Risk
Pain management is frequently audited due to:
- Opioid prescribing regulations.
- High-cost procedures.
- Repetitive injections.
- Frequency limitations.
Practices must comply with:
→ LCD (Local Coverage Determinations
→ NCD (National Coverage Determinations)
→ OIG guidelines
→ Payer-specific policies
Non-compliance may lead to penalties, repayments, or legal risk.
6. Administrative Burden
The complexity of billing rules increases administrative workload. Staff often spend significant time on: appeals management, authorization follow-ups, documentation corrections, and denial tracking.
This reduces clinical productivity and increases operational costs.
7. Patient Payment Challenges
With rising deductibles and out-of-pocket expenses, patient collections have become increasingly difficult.
Practices face challenges such as:
- Delayed patient payments.
- Confusion over coverage.
- Financial hardship cases.
- Payment plan management.
Poor front-end financial counseling can negatively impact revenue cycles.
Pain management billing is not just about submitting claims… it requires regulatory awareness, coding precision, authorization management, and strong documentation practices.
Without a specialized billing strategy or outsourcing pain management medical billing company, practices may experience increased denials, delayed reimbursements, and compliance risks.
Best Practices to Improve Reimbursement in Pain Management Medical Billing

To enhance the reimbursement, process enhancement, training, and technology are needed.
→ Introduce Billing Practice Audits
Regular audits assist in exposing coding errors and lapses in compliance. Studies reveal that most claim denials can be avoided through effective documentation and review reports.
→ Invest in Coding Expertise
Specialty-trained coders from pain management medical billing companies are aware of procedures for pain management medical billing guidelines and payer requirements.
→ Improve Front-End Processes
More than half of the claim rejections can be prevented with proper registration of patients and their eligibility.
→ Automation and Claim Scrubbing Tools
The billing system should be automated, and coding and data errors should be identified before the submission of claims.
→ Track Denial Trends
Denial data monitoring enables practices to correct root causes, and over time, they will have a higher clean claim rate.
Such practices that implement optimal billing processes and professional billing assistance may see an improvement in revenue collection and a cut in administrative expenditure.
Ready to Increase Revenue? Outsource Pain Management Billing to Health & Billing!

In-house pain management billing can be time-consuming, less beneficial, and expensive for your practice…. With Health & Billing as your outsourced pain management billing partner, you can take a sigh of relief.
Our services are guaranteed to provide you with:
- Reduce claim denials
- Enhance the reimbursement speed.
- Provide coding compliance and accuracy.
- Minimized administrative workload.
- Ensure general growth in revenue performance.
Pay more attention to patients and leave the pain management medical billing, and coding revenue cycle management to the expert team of Health & Billing professionals! Contact Now, Book a FREE Consultation with us!
FAQs
What is complicated about the billing of pain management?
The billing pain management implies various processes, the necessity of documenting a large number of records, and prior authorizations. They make coding more complex and increase the risks of denials as compared to general medical billing.
How often should pain management billing be audited?
The majority of experts suggest that a billing audit should be performed at least every quarter or at least once every six months.
What are the common errors in pain management billing?
Some common errors include:
- Wrong CPT codes
- Missing modifiers
- Incomplete documentation
- Not getting prior authorization for procedures.
Should you outsource your pain management billing?
Outsourcing pain management medical billing and coding has several benefits to various practices since a pain management medical billing company produces a better quality of claims, lowering denials, and improving care collection rates.































 Operating a small medical practice can be a lot of work, especially when taking care of patients and other administrative responsibilities!
Operating a small medical practice can be a lot of work, especially when taking care of patients and other administrative responsibilities!