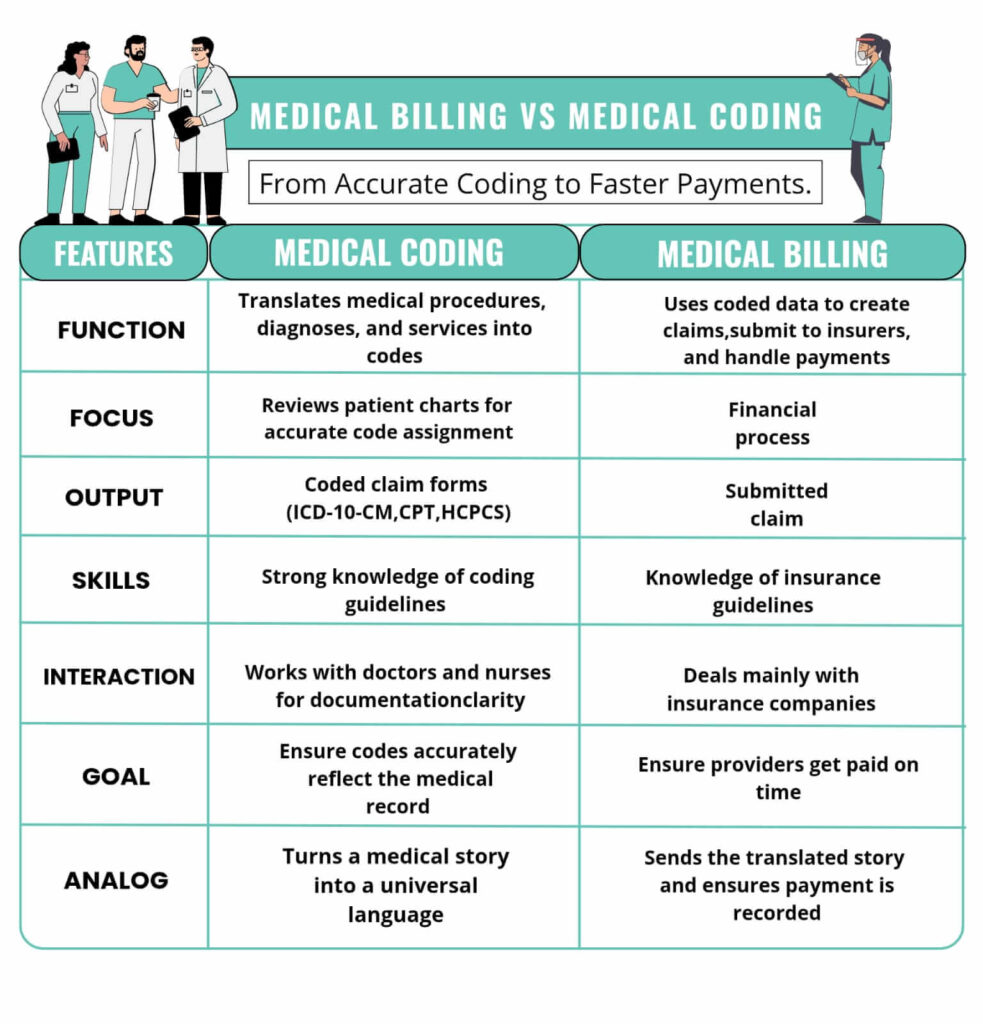
Urgent care facilities play a critical role in the modern healthcare system due to their commitment to offering fast and convenient treatment for non-life-threatening conditions. Patients do not need an appointment to utilize a service at urgent care, because, as the name suggests, they are usually quick and accessible, catering to an injury or accident.
However, the scope of service is marred by unique challenges pertaining to the billing system. A healthcare provider may expect the rightful payment after rendering care; however, patient influx and a wide variety of insurance plans increase the probability of claim denials and delayed payments.
This guide breaks down urgent care medical billing and coding in simple terms to help you understand the process, avoid common mistakes, and improve overall financial performance.
What is Urgent Care in Medical Billing?

Urgent care refers to outpatient services provided by a healthcare facility for immediate but non-emergency medical needs. These typically include treatment of minor injuries, infections, flu symptoms, sprains, cuts, and burns. Performing diagnostic tests like X-rays or lab work also falls under the category.
In medical billing, urgent care entails the specialized process of coding, documenting, and submitting claims for medical services rendered. Because patient visits are usually high-volume and without appointments, billing is ought to be handled quickly and accurately.
What Makes Urgent Care Billing Unique!
Urgent care centers differ from family medicine or emergency departments. They treat a high volume of walk-ins. Also, the unscheduled patients with a variety of minor injuries, infections, diagnostics, and procedures. Henc,e that all leads to a complex mix of billing requirements and compliance rules.
Key characteristics:
- High patient turnover with a large mix of services.
- Frequent use of Evaluation & Management (E/M) codes and procedure codes.
- Distinct place of service (POS) code for urgent care (typically POS 20).
How Urgent Care Medical Billing Differs from Other Medical Billing Models?
The urgent care billing process is different from other healthcare billing models in several important ways. These differences are usually ascribed to the high influx of walk-in patients and rapid documentation. The claims for each urgent care bill must be processed the same day due to the aforementioned factors.
Other types of billing, such as emergency room or primary care billing involves higher reimbursement rates and flexibility from insurance companies. Meanwhile, payers usually pay close attention to urgent care claims to make sure the visit was appropriate for an urgent care setting. Moreover, the provider must ensure patient information, including insurance verification and demographic is accurate at the time of check-in.
Billing systems in urgent care use specific coding systems to translate patient services into standardized universal numerical codes, which are then used for accurate insurance reimbursement and minimal claim denials.
Urgent Care Medical Billing Process: Step-by-Step Overview

Billing for urgent care may appear frightening to healthcare providers due to the increased probability of errors despite rendering optimal patient care.
Thus, sticking to a step-by-step process is the best bet in preventing otherwise common errors in billing.
- Patient Registration and Insurance Verification: The front-desk staff collects patient information, confirms insurance coverage, and identifies copays and deductibles. If done accurately, this stage sets the foundation for clean claims.
- Clinical Documentation and Coding: There are special codes for services rendered to the patient at urgent care, depending on the visit, diagnosis, and procedure. These help in insurance reimbursement after the patient is billed.
- Claim Submission: Once coding is completed and the service is well-documented, claims are submitted to insurance companies.
- Payment Posting and Adjustments: After the claim is submitted, payers process it by applying the allowed amount to determine what they will pay versus what the patient owes.
- Patient Billing and Follow-up: Finally, patients receive statements for their remaining balance after clearance from the payers. Billing staff may also follow up on unpaid claims or denied services at this stage.
Urgent Care Billing Guidelines and Compliance Requirements
The billing of urgent care should be guided by the strict guidelines to guarantee accuracy, regulations, and reimbursement in time. Since the urgent care centers deal with large volumes of patients and comprise diverse services, it is necessary to ensure that they have adequate billing practices that prevent claims rejection, audits, and financial fines.
Among the most important needs in emergency care billing, proper and complete clinical records must be mentioned. The providers are required to effectively record the chief complaint of the patient, his or her medical history, physical examination, diagnostic tests, treatments, and medical decision-making.
This documentation is required to support the Evaluation and Management (E/M) level billed and to support medical necessity.
The urgent care claims should also adhere to the payer-specific billing regulations, such as Medicare, Medicaid and the commercial insurance regulations.
The CPT, ICD-10, and HCPS codes should be used properly, and the proper Place of Service (POS) code should be used…
When there is a wrong coding, a lack of a modifier, or unsubsidized services, claim rejections or downcoding can occur.

The adherence to the HIPAA requirements should also be followed during the urgent care billing process. The information on patients should be treated with care when registering patients, coding and submitting claims, and posting payments to avoid data leakage and legal liability.
Moreover, the urgent care facilities are to introduce in-house compliance measures, routine practice audits of its facilities, and continuous clinical and billing personnel training.
These are measures that can determine the mistakes made at early stages, ensure that the standards of regulation are met, and the flow of revenues is regular.
Adhering to the set rules of billing and ensuring the utmost rate of compliance, urgent care centers have a chance of minimizing denials, enhancing payment and collection accuracy, and avoiding regulatory and financial risks to the practice.
Common Challenges in Urgent Care Billing
There are several challenges that come with medical billing in urgent care centers, which can impact revenue if not managed properly.
→ Incorrect Patient Information: In case of incomplete or incorrect patient information during check-in, such as misspelled names, incorrect insurance details, or outdated coverage often leads to claim denials.
→ Coding Errors: Due to the high volume of patients at urgent care, documentation may lack detail, making it harder to code accurately.
→ Claim Denials and Underpayments: One of the most common issues in urgent care billing is due to stricter insurance policies at the payer’s end.
Best Practices to Improve Urgent Care Billing Performance

- Front-end Accuracy: The billing performance for urgent care can largely be improved by strengthening front-end processes.
Accurate documentation and verifying insurance eligibility during patient check-in help prevent claim denials and delayed payments.
- Staff Training: The facility staff must be regularly trained in their respective specialty, such as the billing and coding teams, who must be accustomed to urgent care coding rules and payer guidelines.
- Claims Review: Providers should also review claims before submission to limit rejections or completely prevent them by catching errors early.
- Timely Follow-ups: Follow-ups are crucial in medical billing, especially when insurance is involved. There should be a dedicated team to track denials and subsequently appeal them to prevent revenue loss.
The Role of Revenue Cycle Management in Urgent Care
Revenue Cycle Management (RCM) plays a vital role in urgent care operations. It refers to the process providers use to track, code, bill, and collect payment for the care they provide. It essentially covers every step from patient registration to final payment.
Effective revenue cycle management for urgent care entails accurate submission of claims after a service is provided and efficient collection of patient balances. It also helps urgent care facilities identify underpayments and billing errors.
Urgent care revenue cycle management:
→ Ensures Accurate Patient Registration. Verifies insurance eligibility, demographic details, and copays at check-in to prevent claim errors and denials.
→ Supports Proper Coding and Documentation. Aligns CPT, ICD-10, and HCPCS codes with clinical documentation to justify medical necessity and appropriate reimbursement.
→ Improves Claim Submission Accuracy. Reduces rejections by submitting clean, compliant claims the first time.
→ Manages Denials and Appeals Efficiently. Identifies denial trends, corrects errors, and submits timely appeals to recover lost revenue.
→ Optimizes Cash Flow. Speeds up reimbursement cycles and minimizes delayed or missed payments.
→ Tracks Underpayments and Adjustments. Ensures payers reimburse according to contracted rates and flags discrepancies early.
→ Enhances Compliance. Maintains adherence to Medicare, Medicaid, commercial payer, and HIPAA regulations.
→ Reduces Administrative Burden. Streamlines billing workflows so clinical staff can focus on patient care.
→ Provides Financial Insights. Uses reporting and analytics to monitor revenue performance and identify improvement areas.
→ Supports Long-Term Growth. Creates a scalable billing infrastructure that sustains financial stability in high-volume urgent care settings.
Outsource Your Urgent Care Medical Billing to Health & Billing!
More and more medical practices are choosing to outsource urgent care rcm and billing services in order to reduce administrative burden and improve results. It is a fitting option for when billing and coding processes interfere with patient care.
As urgent care billing experts, Health & Billing offers outsourcing medical billing services in Florida so providers can ease off from managing insurance rules, requirements, and denials. You can also cut down on staffing costs and eliminate the need for their training, software maintenance, and compliance monitoring by delegating it all to us.
Why Choose Health & Billing for Outsourcing Urgent Care Billing Services?
Health & Billing harbors a specialized team of experienced billing professionals who understand the fast-paced nature of urgent care operations. We offer customized solutions for minimal claim denials, improved collections, and rigorous compliance.
Every medical practice, especially urgent care centers, seeks financial stability and efficient RCM. By partnering with Health & Billing, urgent care centers gain reliable billing support, improved cash flow, and peace of mind knowing their revenue cycle is in expert hands!!!
Urgent care medical billing doesn’t have to be complicated anymore. Reach out to Health & Billing to learn how our specialized billing services can support your growth and success.
FAQs
What makes urgent care billing different from other medical billing?
Urgent care billing is fast-paced due to high-volume of patients and rapid documentation. The visits are relatively shorter and without appointments than in primary care or ER settings.
Why is urgent care billing so complicated?
Each patient visiting an urgent care clinic has a different insurance plan, thus coding and documentation need to be accurate.
How to improve urgent care billing accuracy?
Verifying insurance, accurately documenting patient information, using correct codes for services rendered, reviewing claims, and following up promptly.
Why do urgent care claims get denied?
Denials often happen due to incorrect patient information, coding errors, missing documentation, or ineligible insurance coverage.