 Operating a small medical practice can be a lot of work, especially when taking care of patients and other administrative responsibilities!
Operating a small medical practice can be a lot of work, especially when taking care of patients and other administrative responsibilities!
One of the most difficult tasks is to find a way to handle billing and process insurance claims. Insufficient handling of accounts receivable can result in delayed payments, cash flow problems, and more stress for patients, staff members, and other involved parties.
This is where the right medical billing software for small businesses can make all the difference. By streamlining workflows, reducing human errors, and accelerating collections, these solutions help practices maintain financial stability while freeing up more time for patient care, the true heart of any medical business.
This article focuses on the most appropriate and efficient medical billing software for small practices. These software solutions help the healthcare billing system to become more efficient and save on time and other administrative tasks.
Key Features to Look for in Medical Billing Software for Small Practices
When choosing the best medical billing software for a healthcare billing system, it’s essential to focus on the features that matter most to small practices: those that streamline workflows, reduce errors, and improve overall efficiency.
The best medical billing software combines automation, compliance, and usability, ensuring financial health while freeing up valuable time for patient care.
| Features of Medical Billing Software for Small Businesses | Why It Matters for Small Practices? |
| Error Checking & Claim Scrubbing | Reduces claim denials by catching missing fields, coding mistakes, or mismatched insurance details before submission. |
| Real-Time Insurance Eligibility Verification | Instantly verifies patient coverage, co-pays, and deductibles, minimizing rejections and improving patient trust. |
| Integrated EHR, Practice Management & Scheduling | Eliminates duplication by ensuring patient data flows seamlessly from scheduling to billing. Critical for efficiency in small teams. |
| Compliance & Data Security | HIPAA compliance, secure submissions, backups, and audit logs protect sensitive patient and financial data. |
| Robust Dashboard & Reporting | Tracks claims status, AR days, and revenue trends, helping providers quickly spot financial bottlenecks. |
| Patient Portals & Flexible Payment Options | Improves collections by offering online billing access, payment reminders, and installment options for patients. |
| Transparent Pricing Structure | Provides clarity on subscription, per-claim, or per-provider costs, avoiding hidden fees for integrations or support. |
| User Experience, Support & Training | A clean UI, short learning curve, and responsive customer support reduce staff frustration and downtime. |
| Scalability & Specialty Billing Support | Ensures the system can adapt as the practice grows, handling multiple specialties, providers, or locations. |
| Advanced Analytics & Insights | Helps identify payer patterns, patient payment delays, and denial trends to refine long-term financial performance. |
Top 10 Best Medical Billing Software for Small Businesses
The below discussed 10 software systems have been established in the market and meet most of the above-mentioned features.
1. eClinicalWorks


eClinicalWorks is an AI-powered medical billing software for small businesses. It has an interoperable system that interconnects billing and clinical/patient engagement systems. Its analysis applications assist in monitoring such KPIs as days in A/R and denial rates.
Advanced Features
- Comprehensive Suite: Provides EHR, patient interaction, and billing.
- Interoperability: Interoperable with networks, like Carequality.
- Voice-Based Documentation: AI-assisted voice-based documentation option.
- Population Health Management: Applicable to value-based care.
Potential Trade-offs
- User Interface: May be cluttered for new visitors.
2. DrChrono
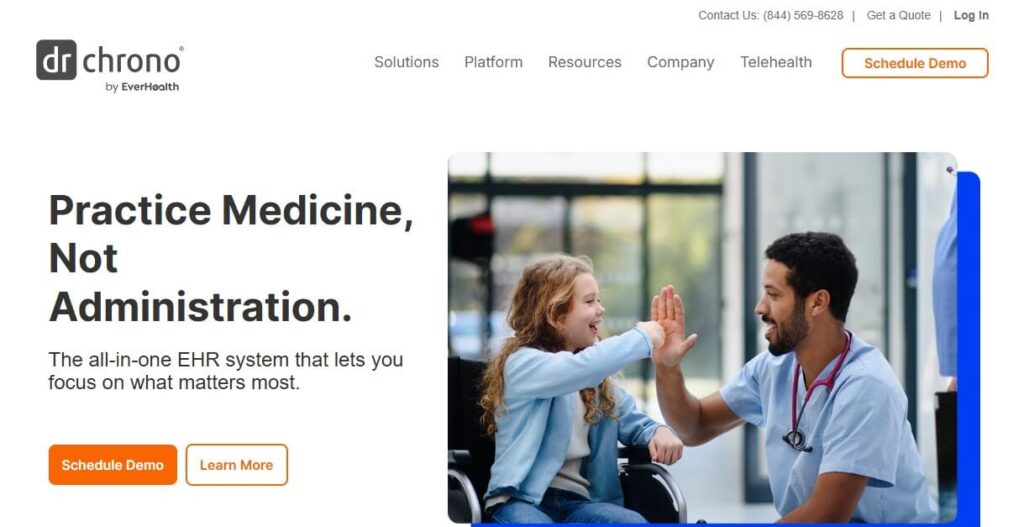
DrChrono is a modern, mobile-first billing system. It contains the scheduling, patient engagement, and EHR features. It has a clean interface and customizable billing workflows, with the help of which small practices reduce their errors and receive reimbursement faster.
Advanced Features
- Mobile-First Design: Official Apple Mobility partner, it also works on iPads and iPhones.
- Real-Time Checking of Eligibility: Minimises claim denials.
- Workflow customisation: Dynamic to practice size.
- Designed for 20+ Specialties.
- Built-in Telehealth and eRx: Makes recent practice convenient.
Potential Trade-offs
- Poor Advanced Analytics: Reporting capabilities are proficient, yet not as comprehensive as those of other competitors.
- Response Times Support: Some customers say that they received slower customer support at certain peak times.
3. Kareo; Now Tebra
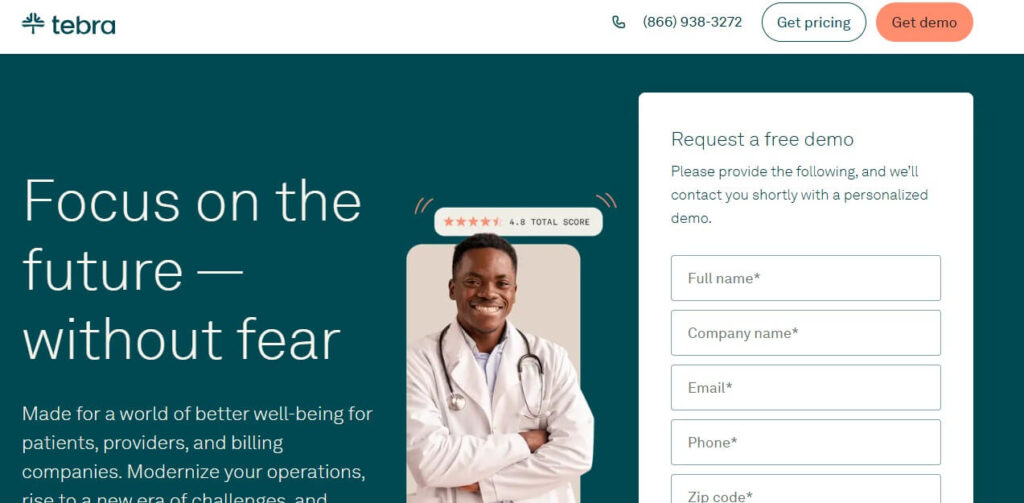
Tebra is among the most used small and single practice solutions. It is easy to use. Kareo consists of claims management, patient statements, collections tracking, and analytics dashboards.
Advanced Features
- Cloud-Based Solution: There is no requirement for on-site servers.
- Real-time Tracking on Claims: Easy trackers.
- Patient-Friendly Statements: Patient communication made easy.
Potential Trade-offs
- Limited Customisation Large Practices: It best fits small to mid-sized practices.
- Infrequent Glitches: Users complain of technical issues with the software.
4. AdvancedMD
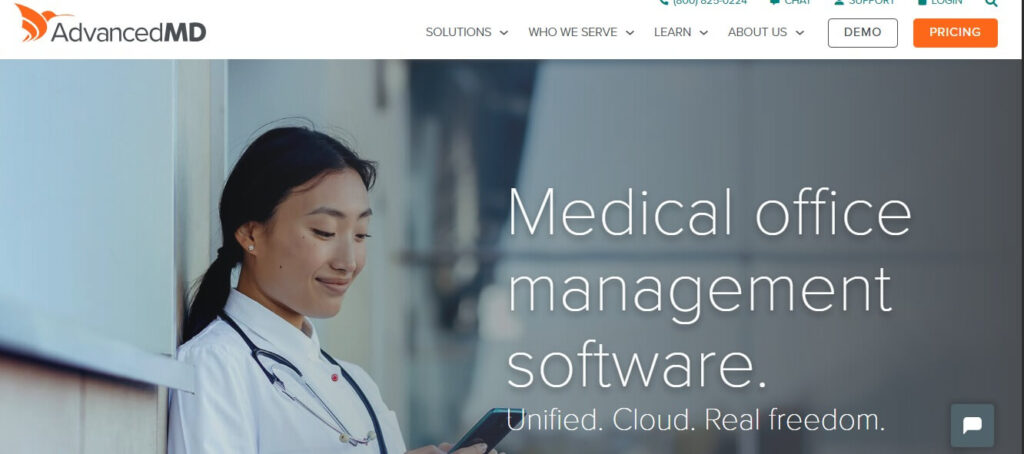
AdvancedMD is a powerful, scaled-out healthcare billing system that growing practices require. Its end-to-end platform includes an area of claim scrubbing, RCM services, and business intelligence tools. AdvancedMD is the best choice when you require detailed reporting and automation.
Advanced Features
- Scalable Platform: Ideal where there are many locations in practice.
- End-to-End RCM Tools: These include scheduling, billing, reporting, and patient engagement.
- High Automation: Auto-reminders, claims scrubbing, and payment posting.
- Business Intelligence Dashboard: Real-time financial insights.
Potential Trade-offs
- Heavy Learning Curve: Time-consuming to learn since it is in-depth.
- Price: The high price point in comparison with small-practice solutions.
5. CentralReach
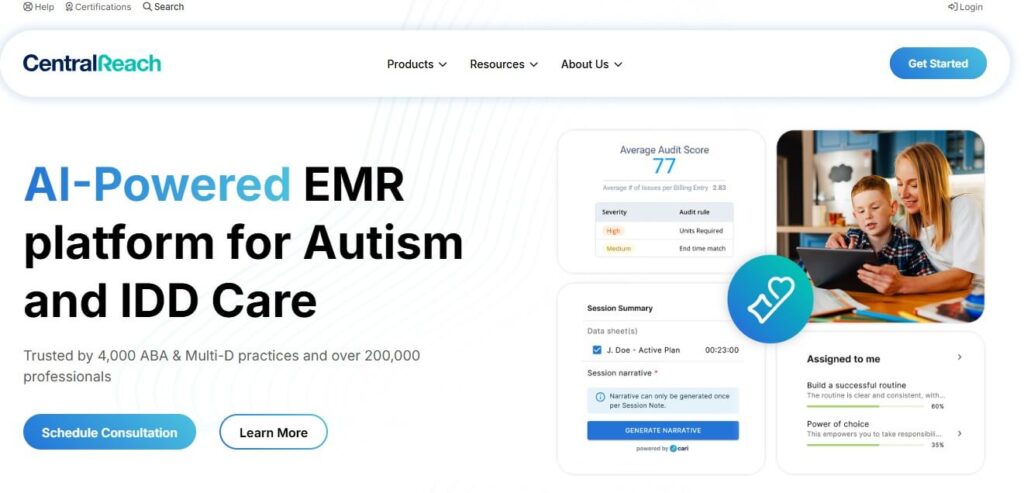
CentralReach is AI-powered, focuses on the practice management of ABA (Applied Behaviour Analysis). In the case of therapy and behavioural health clinics, their billing system will combine the scheduling, data collection, and insurance claims, ensuring the revenue cycle management is flawless.
Advanced Features
- ABA & IDD Specialisation: This is an ABA-focused treatment for autism that is purpose-built as well.
- End-to-End Billing: Submission of claims, scrubbing, tracking, and denial administration.
- Clinical Documentation: Auto-graphing, custom forms, and offline data collection.
- Analytics & Reporting: KPIs, financial performance, and utilisation.
- Client Portal: Caregivers can look at the invoices and session history.
Potential Trade-offs
- Increase in Cost of Scale: Price increases with employees, destinations, and extras.
- Steep Learning Curve: It takes time to train and set up.
6. AthenaCollector (Athenahealth)
AthenaCollector is famous because of its AI-powered processes that enhance the accuracy and speed of claims. It has inbuilt rules engines, real-time claim tracking, and reporting dashboards to assist small practices in increasing collections.
Advanced Features
- Rule-Based Claim Scrubbing: Large first-pass acceptance rate.
- Denial Management Tools: Tracks denials so that they can be reasserted successfully.
- Built-in Patient Communication: SMS and email messages.
Potential Trade-offs
- Personalisation Weakness: Not as flexible as competitors.
- Revenue Sharing Model: Some practices do not like percentage-based pricing.
7. NextGen Office
The cloud solution of NextGen can be customised for numerous specialities. It consists of templates that can be customized, claim scrubbing, and integrating a patient portal. Useful when the practices require specialty-specific features and scalability.
Advanced Features
- Specialty-focused designs: Tailored designs for many specialities.
- Intense Interoperability: Electronic labs, pharmacies, and other EHRs.
- Beyond Reporting and Analytics: Best in data-driven decision making.
- Revenue Cycle Management Support: Provides outsourced billing and software
- Designed for small to mid-sized to enterprise-level practices.
Potential Trade-offs
- Difficult to set up: Staff must be trained on the full usage of its features.
- Pricing Transparency: The pricing may change as per the customisation requirements.
8. CureMD
CureMD provides an all-in-one cloud-based billing system that interfaces with EHR and practice management solutions. It has an intuitive dashboard with real-time claim status, automated eligibility checking features, and denial management capabilities, which are less complicated to increase first-pass acceptance rates.
Advanced Features
- EHR + Billing: This is an integrated practice management, EHR, and billing platform.
- AI-Based Scrubbing of Claims: Reduces refusals and rejections.
- Patient Portal and Payments: Patients can access and pay bills online.
- HIPAA/ICO-10 compliant.
Potential Trade-offs
- Learning Curve: The interface is so full of features that it might require some time to get oriented.
- Price: Moderately high prices in contrast to other smaller competitors.
9. PracticeSuite
PracticeSuite is a low-cost and feature-packed platform that grows with your practice. It consists of scheduling appointments, claims, and payments, and custom reporting, which is the most suitable medical billing software for small businesses with a tight budget.
Advanced Features
- End-to-End Revenue Management: Scheduling, billing, and reporting.
- Multi-Location Support: Fits the expanding practice.
- Customizable Templates: Specialty-specific customisation.
- Price: Clear strategy for various sizes of practices.
Potential Trade-offs
- Poor Advanced Analytics: Good reporting, not so powerful as NextGen or Advanced.
10. EZClaim
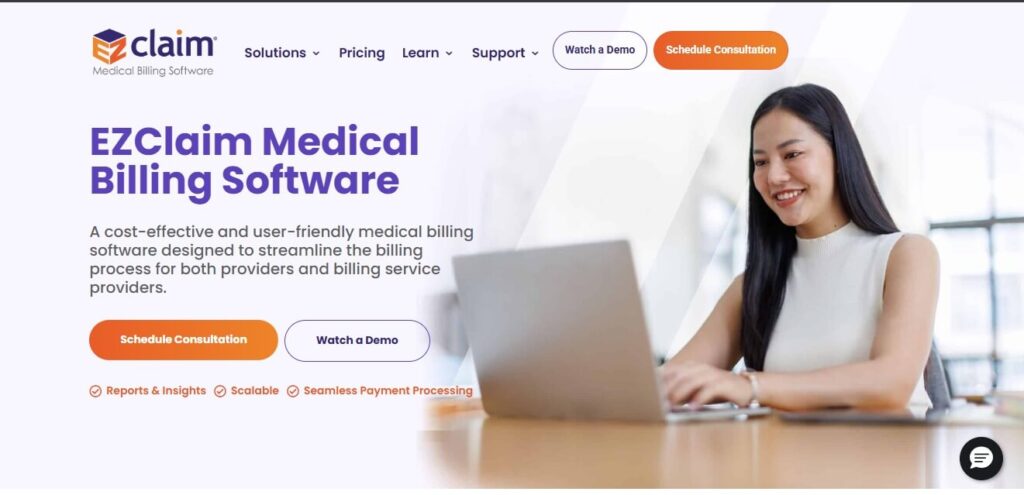
EZClaim is a cost-effective and user-friendly medical billing software for small practices. It serves as an ideal entry point for small practices for a healthcare billing system. Its low-end model is based on quick claims type submission, uploading of payment, and minimal reporting without excessive complexity of operations.
Advanced Features
- Simple Interface: The simple interface is user-friendly.
- Low Prices: Suitable for small practices and individual providers.
- Portable Deployment: Cloud and desktop solutions at hand.
Potential Trade-offs
- Minimal Capabilities on Large Practices: Lacks complex automation instruments.
- Simple Reporting: Not the best suited to complex financial practices.
Dashboard & Reporting: What Small Practices Should Look For?
When evaluating medical billing software, the dashboard should give small practices a clear, real-time snapshot of their financial and operational health.
A well-designed reporting system highlights key metrics, identifies problem areas, and supports data-driven decision-making. Look for dashboards that include:
→ Claims Overview: Track submitted, denied, and paid claims at a glance.
→ Denial Analysis: Identify the most common denial reasons to quickly address recurring issues.
→ Accounts Receivable (AR) Days: Break down AR by payer and service type for more precise follow-up.
→ Patient Receivables Aging: Monitor outstanding balances across 30/60/90+ days to improve collections.
→ Revenue Insights: View revenue trends by provider, specialty, or location (if applicable).
→ Monthly & Year-to-Date Trends: Spot seasonal fluctuations and forecast future revenue.
→ Payer Mix & Performance: Compare insurers to see which delay payments or generate higher denial rates.
→ Task & Workflow Monitoring: Stay on top of unbilled services, pending claims, appeals, or bottlenecks.
→ Visual Reporting Tools: Use graphs, pie charts, color coding (green = good, red = issue), and drill-down capabilities for deeper analysis.
How to Select the Best Medical Billing Software for Small Practices?
The planned process for selecting medical billing services for small practices will allow for avoiding regrets and a successful transition. You should:
1. Be clear in your requirements:
- Number of providers/users
- Specialities (if any)
- Monthly claim volume
2. Current systems (EHR/Scheduling) and integration requirements:
- Set budget expectations
- Upfront vs recurring fees
3. Select 2-3 solutions and make a comparison:
- Request demo sessions
- Inquire about dashboard previews, reporting
- Inquire about onboarding and migrations
4. Check: How difficult is the transfer of data in the existing system?
- Training for staff
- Check compliance and data security
- HIPAA (or locally/ GDPR or a regulatory health data law)
- Encryption, audit logs, and backups
5. Pilot phase:
- Pilot on a small scale (one provider or one location).
- Track important indicators: denial rate, days in AR, and turn-time made on claim.
6. Measure and optimize continuously:
- Dashboard to detect areas of problems.
- Frequent employee and provider feedback.
Choose Convenience, Choose Health & Billing!
Or you can choose an expert medical billing services provider company, having complete knowledge and information about healthcare billing systems and medical billing software for small businesses.
Here’s what you gain when you choose Health & Billing:
Customized Solutions: Select standalone medical billing software or a complete billing service, just what your practice’s needs!
Transparent, Affordable Packages: Clear pricing designed for individual providers and small clinics, no hidden fees, no surprises for you!
Actionable Insights at Your Fingertips: Instantly track claim status, denials, AR days, and patient balances to spot delays and recover your revenue faster.
Patient-Friendly Technology: We offer online portals, automated notifications, and flexible payment plans to improve patient satisfaction and collections.
Compliance & Security Guaranteed: Stay HIPAA-compliant with secure claims submission, data protection, and reliable backups.
Seamless Transition & Ongoing Support: From onboarding to training, our responsive local support ensures you never face billing challenges alone.
With the right partner, your practice can reduce stress, speed up payments, and free more time for what matters most: your patients!
Bottom Line
One of the best choices that a small practice can make is to pick medical billing services that know about healthcare billing systems and the best medical billing software for small businesses. The right system translates to fewer refusals, quicker payments, more time to attend to patients, and eventually a healthier bottom line.
It can make sure you receive a system that not just works but makes your practice faster in terms of its financial well-being, with consideration of the features, comparisons, dashboards, pricing transparency, and support for the other strategies employed by the competitors.

















![{"type":"elementor","siteurl":"https://healthandbilling.com/wp-json/","elements":[{"id":"903b684","elType":"widget","isInner":false,"isLocked":false,"settings":{"image":{"url":"https://healthandbilling.com/wp-content/uploads/2025/09/124061.jpg","id":13039,"alt":"","source":"library","size":""},"animation_delay":"0","el_class":"img-fluid","wrap_el_class":"content-6-img right-column","wrap_el_classes":"content-6-img pl-0","_padding":{"unit":"px","top":"0","right":"0","bottom":"0","left":"0","isLinked":true},"thumbnail_custom_dimension":{"width":"500","height":"1000"},"image_alt_text":"","thumbnail_size":"large","image_rounded_cornors":"","image_alignment":"","image_alignment_tablet":"","image_alignment_mobile":"","link":{"url":"","is_external":"","nofollow":"","custom_attributes":""},"animation":"","el_classes":"","_title":"","_margin":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_margin_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_margin_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_element_width":"","_element_width_tablet":"","_element_width_mobile":"","_element_custom_width":{"unit":"%","size":"","sizes":[]},"_element_custom_width_tablet":{"unit":"px","size":"","sizes":[]},"_element_custom_width_mobile":{"unit":"px","size":"","sizes":[]},"_grid_column":"","_grid_column_tablet":"","_grid_column_mobile":"","_grid_column_custom":"","_grid_column_custom_tablet":"","_grid_column_custom_mobile":"","_grid_row":"","_grid_row_tablet":"","_grid_row_mobile":"","_grid_row_custom":"","_grid_row_custom_tablet":"","_grid_row_custom_mobile":"","_flex_align_self":"","_flex_align_self_tablet":"","_flex_align_self_mobile":"","_flex_order":"","_flex_order_tablet":"","_flex_order_mobile":"","_flex_order_custom":"","_flex_order_custom_tablet":"","_flex_order_custom_mobile":"","_flex_size":"","_flex_size_tablet":"","_flex_size_mobile":"","_flex_grow":1,"_flex_grow_tablet":"","_flex_grow_mobile":"","_flex_shrink":1,"_flex_shrink_tablet":"","_flex_shrink_mobile":"","_element_vertical_align":"","_element_vertical_align_tablet":"","_element_vertical_align_mobile":"","_position":"","_offset_orientation_h":"start","_offset_x":{"unit":"px","size":0,"sizes":[]},"_offset_x_tablet":{"unit":"px","size":"","sizes":[]},"_offset_x_mobile":{"unit":"px","size":"","sizes":[]},"_offset_x_end":{"unit":"px","size":0,"sizes":[]},"_offset_x_end_tablet":{"unit":"px","size":"","sizes":[]},"_offset_x_end_mobile":{"unit":"px","size":"","sizes":[]},"_offset_orientation_v":"start","_offset_y":{"unit":"px","size":0,"sizes":[]},"_offset_y_tablet":{"unit":"px","size":"","sizes":[]},"_offset_y_mobile":{"unit":"px","size":"","sizes":[]},"_offset_y_end":{"unit":"px","size":0,"sizes":[]},"_offset_y_end_tablet":{"unit":"px","size":"","sizes":[]},"_offset_y_end_mobile":{"unit":"px","size":"","sizes":[]},"_z_index":"","_z_index_tablet":"","_z_index_mobile":"","_element_id":"","_css_classes":"","_element_cache":"","_animation":"","_animation_tablet":"","_animation_mobile":"","animation_duration":"","_animation_delay":"","_transform_rotate_popover":"","_transform_rotateZ_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateZ_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateZ_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotate_3d":"","_transform_rotateX_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateX_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateX_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateY_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_perspective_effect":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translate_popover":"","_transform_translateX_effect":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scale_popover":"","_transform_keep_proportions":"yes","_transform_scale_effect":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_skew_popover":"","_transform_skewX_effect":{"unit":"px","size":"","sizes":[]},"_transform_skewX_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewX_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect":{"unit":"px","size":"","sizes":[]},"_transform_skewY_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_flipX_effect":"","_transform_flipY_effect":"","_transform_rotate_popover_hover":"","_transform_rotateZ_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateZ_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateZ_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotate_3d_hover":"","_transform_rotateX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateX_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateX_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateY_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_perspective_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translate_popover_hover":"","_transform_translateX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scale_popover_hover":"","_transform_keep_proportions_hover":"yes","_transform_scale_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_skew_popover_hover":"","_transform_skewX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_skewX_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewX_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_skewY_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_flipX_effect_hover":"","_transform_flipY_effect_hover":"","_transform_transition_hover":{"unit":"px","size":"","sizes":[]},"motion_fx_transform_x_anchor_point":"","motion_fx_transform_x_anchor_point_tablet":"","motion_fx_transform_x_anchor_point_mobile":"","motion_fx_transform_y_anchor_point":"","motion_fx_transform_y_anchor_point_tablet":"","motion_fx_transform_y_anchor_point_mobile":"","_background_background":"","_background_color":"","_background_color_stop":{"unit":"%","size":0,"sizes":[]},"_background_color_stop_tablet":{"unit":"%"},"_background_color_stop_mobile":{"unit":"%"},"_background_color_b":"#f2295b","_background_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_background_color_b_stop_tablet":{"unit":"%"},"_background_color_b_stop_mobile":{"unit":"%"},"_background_gradient_type":"linear","_background_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_background_gradient_angle_tablet":{"unit":"deg"},"_background_gradient_angle_mobile":{"unit":"deg"},"_background_gradient_position":"center center","_background_gradient_position_tablet":"","_background_gradient_position_mobile":"","_background_image":{"url":"","id":"","size":""},"_background_image_tablet":{"url":"","id":"","size":""},"_background_image_mobile":{"url":"","id":"","size":""},"_background_position":"","_background_position_tablet":"","_background_position_mobile":"","_background_xpos":{"unit":"px","size":0,"sizes":[]},"_background_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_ypos":{"unit":"px","size":0,"sizes":[]},"_background_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_attachment":"","_background_repeat":"","_background_repeat_tablet":"","_background_repeat_mobile":"","_background_size":"","_background_size_tablet":"","_background_size_mobile":"","_background_bg_width":{"unit":"%","size":100,"sizes":[]},"_background_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_background_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_background_video_link":"","_background_video_start":"","_background_video_end":"","_background_play_once":"","_background_play_on_mobile":"","_background_privacy_mode":"","_background_video_fallback":{"url":"","id":"","size":""},"_background_slideshow_gallery":[],"_background_slideshow_loop":"yes","_background_slideshow_slide_duration":5000,"_background_slideshow_slide_transition":"fade","_background_slideshow_transition_duration":500,"_background_slideshow_background_size":"","_background_slideshow_background_size_tablet":"","_background_slideshow_background_size_mobile":"","_background_slideshow_background_position":"","_background_slideshow_background_position_tablet":"","_background_slideshow_background_position_mobile":"","_background_slideshow_lazyload":"","_background_slideshow_ken_burns":"","_background_slideshow_ken_burns_zoom_direction":"in","_background_hover_background":"","_background_hover_color":"","_background_hover_color_stop":{"unit":"%","size":0,"sizes":[]},"_background_hover_color_stop_tablet":{"unit":"%"},"_background_hover_color_stop_mobile":{"unit":"%"},"_background_hover_color_b":"#f2295b","_background_hover_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_background_hover_color_b_stop_tablet":{"unit":"%"},"_background_hover_color_b_stop_mobile":{"unit":"%"},"_background_hover_gradient_type":"linear","_background_hover_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_background_hover_gradient_angle_tablet":{"unit":"deg"},"_background_hover_gradient_angle_mobile":{"unit":"deg"},"_background_hover_gradient_position":"center center","_background_hover_gradient_position_tablet":"","_background_hover_gradient_position_mobile":"","_background_hover_image":{"url":"","id":"","size":""},"_background_hover_image_tablet":{"url":"","id":"","size":""},"_background_hover_image_mobile":{"url":"","id":"","size":""},"_background_hover_position":"","_background_hover_position_tablet":"","_background_hover_position_mobile":"","_background_hover_xpos":{"unit":"px","size":0,"sizes":[]},"_background_hover_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_hover_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_hover_attachment":"","_background_hover_repeat":"","_background_hover_repeat_tablet":"","_background_hover_repeat_mobile":"","_background_hover_size":"","_background_hover_size_tablet":"","_background_hover_size_mobile":"","_background_hover_bg_width":{"unit":"%","size":100,"sizes":[]},"_background_hover_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_background_hover_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_background_hover_video_link":"","_background_hover_video_start":"","_background_hover_video_end":"","_background_hover_play_once":"","_background_hover_play_on_mobile":"","_background_hover_privacy_mode":"","_background_hover_video_fallback":{"url":"","id":"","size":""},"_background_hover_slideshow_gallery":[],"_background_hover_slideshow_loop":"yes","_background_hover_slideshow_slide_duration":5000,"_background_hover_slideshow_slide_transition":"fade","_background_hover_slideshow_transition_duration":500,"_background_hover_slideshow_background_size":"","_background_hover_slideshow_background_size_tablet":"","_background_hover_slideshow_background_size_mobile":"","_background_hover_slideshow_background_position":"","_background_hover_slideshow_background_position_tablet":"","_background_hover_slideshow_background_position_mobile":"","_background_hover_slideshow_lazyload":"","_background_hover_slideshow_ken_burns":"","_background_hover_slideshow_ken_burns_zoom_direction":"in","_background_hover_transition":{"unit":"px","size":"","sizes":[]},"_border_border":"","_border_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_color":"","_border_radius":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_box_shadow_box_shadow_type":"","_box_shadow_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"_box_shadow_box_shadow_position":" ","_border_hover_border":"","_border_hover_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_color":"","_border_radius_hover":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_hover_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_hover_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_box_shadow_hover_box_shadow_type":"","_box_shadow_hover_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"_box_shadow_hover_box_shadow_position":" ","_border_hover_transition":{"unit":"px","size":"","sizes":[]},"_mask_switch":"","_mask_shape":"circle","_mask_image":{"url":"","id":"","size":""},"_mask_image_tablet":{"url":"","id":"","size":""},"_mask_image_mobile":{"url":"","id":"","size":""},"_mask_notice":"","_mask_size":"contain","_mask_size_tablet":"","_mask_size_mobile":"","_mask_size_scale":{"unit":"%","size":100,"sizes":[]},"_mask_size_scale_tablet":{"unit":"px","size":"","sizes":[]},"_mask_size_scale_mobile":{"unit":"px","size":"","sizes":[]},"_mask_position":"center center","_mask_position_tablet":"","_mask_position_mobile":"","_mask_position_x":{"unit":"%","size":0,"sizes":[]},"_mask_position_x_tablet":{"unit":"px","size":"","sizes":[]},"_mask_position_x_mobile":{"unit":"px","size":"","sizes":[]},"_mask_position_y":{"unit":"%","size":0,"sizes":[]},"_mask_position_y_tablet":{"unit":"px","size":"","sizes":[]},"_mask_position_y_mobile":{"unit":"px","size":"","sizes":[]},"_mask_repeat":"no-repeat","_mask_repeat_tablet":"","_mask_repeat_mobile":"","hide_desktop":"","hide_tablet":"","hide_mobile":""},"defaultEditSettings":{"defaultEditRoute":"content"},"elements":[],"widgetType":"powernode-image","htmlCache":"\t\t\n\t\t\t\t\t\r\n\t\t\t\t\t\n\t\t","editSettings":{"defaultEditRoute":"content","panel":{"activeTab":"content","activeSection":"section_image"}}}]}](https://healthandbilling.com/wp-content/uploads/2025/09/process-of-credentialing-1024x711.webp)